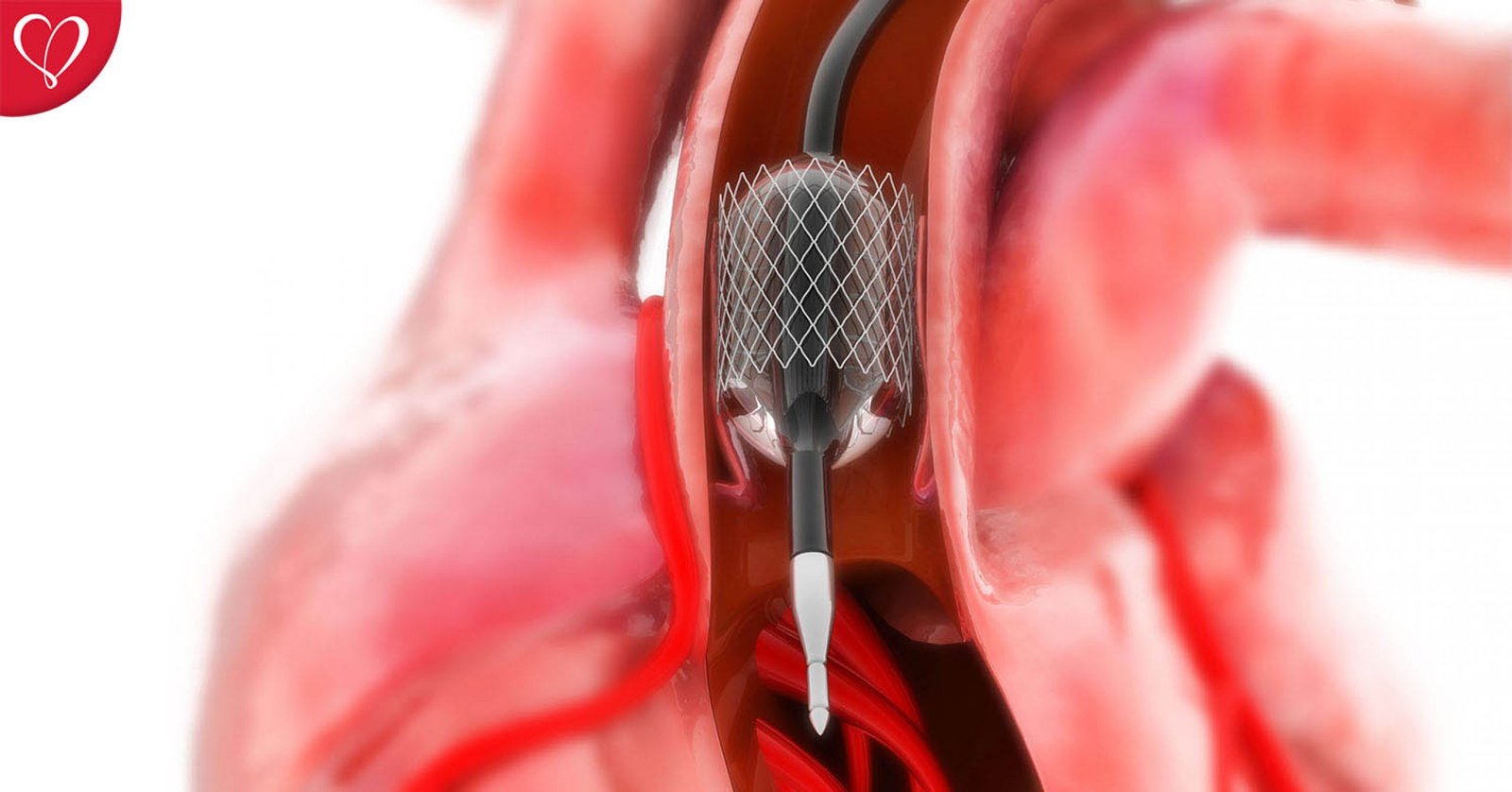
Coronary Angioplasty
What is an Angioplasty?
Grupo Cardiovascular de Tijuana
Haga su cita desde aquí:


Grupo Cardiovascular de Tijuana
Procedures are performed in the cardiac catheterization laboratory, a specialized operating room within a hospital that is equipped to perform diverse hemodynamic procedures.
Patients are generally instructed not to eat or drink anything after midnight the day prior to the procedure.
When patients suffer from Diabetes it is recommended they speak with their primary care doctor in case there is a need to modify insulin dosage, fasting affects the sugar levels in the body.
Talk to your doctor about the medications you are taking, as they may advice you to stop them before the procedure. This is especially important if you are taking blood thinners or antiplatelet agents. It is also very useful to bring a list of your medications so that doctors know exactly what you are taking and in what dosage. It will be necessary to get additional blood tests, an EKG, and a chest X-ray before the procedure.
Once you are admitted to the hospital, a medical team will talk to you and prepare you for the procedure, once in the catheterization lab, you will see large displays around you, and other medical equipment such as heart monitors, and pressure monitors. The patient stays supine on the bed, a type of X ray machine moves around the body while the procedure is being done. Small metal discs called "electrodes" will be placed on your chest. These electrodes have wires called "leads" that connect to an EKG machine.
This machine will monitor your heart rate during the procedure. To prevent infection, the area where the catheter will be inserted will be shaved and sterilized. A needle connected to a tube will be inserted into your arm. This will be the intravenously (IV) access used for different purposes. A mild sedative will be given through this IV to relax you during the procedure. An anesthetic will be injected to numb the area where the catheter will be inserted.
The puncture may hurt a little. After the anesthetic has numbed the area, the cardiologist will make a small incision in the skin. The cardiologist will then identify where the catheter will be inserted and a specialized needle is used to obtain access. The catheter will then be inserted into the artery in your leg, arm, or wrist. Most doctors use the artery in the leg. You should not feel any pain during this part of the procedure.
The catheter then is carefully threaded into the artery and will travel all the way to the heart. The doctors use a video monitor (similar to a television screen) to observe the catheter traveling in real time. When the catheter reaches the blocked artery, a harmless dye (contrast medium) is injected, and doctors take a picture of the coronary arteries (called a "coronary angiogram"). The angiogram allows you to see the size and location of the obstruction. Once the doctor identifies the exact location of the blockage, they insert what is called a "guide wire" through the same artery in the leg and advance it through the blockage. Then, the catheter with the balloon is passed over this guide wire advancing it to the site of the obstruction, where the balloon is inflated. As the balloon dilates, it presses against the atheroma plaque, compressing it against the arterial wall. The balloon is then deflated. Doctors can inflate and deflate the balloon several times. The catheter, guide wire, and deflated balloon are then removed.
The cardiologist may decide a stent is required, this stent is placed at the end of the catheter, above the balloon. When the catheter reaches the site of the obstruction, the balloon is inflated and the stent is opened. Once the stent is open, the balloon is deflated and the catheter, guidewire, and deflated balloon are removed, leaving the stent in place to keep the artery open. The stent will remain inside the patient’s body permanently. At the end of the procedure, the site where the catheter was inserted will be firmly pressed to stop any possible blood loss and a surgical packaging will be placed.
The procedure generally takes between an hour and a half to two and a half hours, generally patients must spend the night in the hospital and will feel sleepy until the effects of the sedative wear off. The nursing staff will monitor the patient at night to make sure heart rate and blood pressure remain normal.
Grupo Cardiovascular de Tijuana
Haga su cita desde aquí:
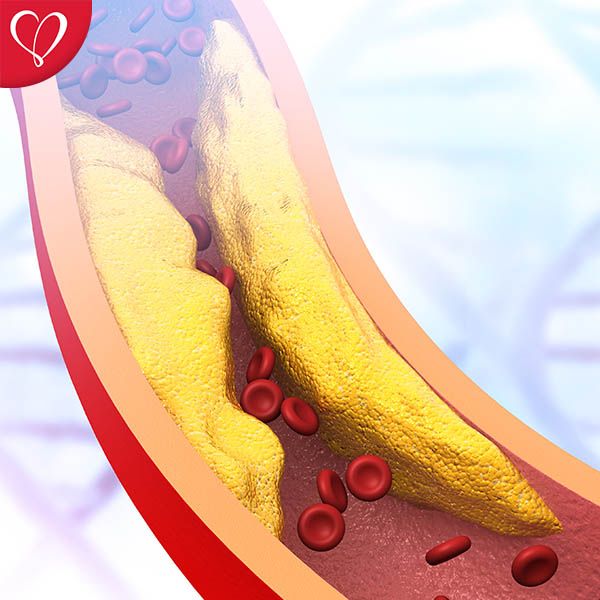
What happens after the procedure?
After leaving the hospital, the following is adviced; do not drive a vehicle, do not soak in a bath, do not smoke for at least a couple of days after the procedure, you should drink plenty of fluids. It is not recommended to walk or stand for long periods of time a few days after the procedure. If you received a stent, no strenuous exercise for at least 30 days. Patients with stents will also have to take antiplatelet agents for the rest of their lives.
About 35 - 40 % of patients who undergo balloon angioplasty are at risk for additional obstructions in the treated area. This is called "restenosis." Restenosis typically occurs within six months of balloon angioplasty. The arteries in which the stents have been placed can also close again. Restenosis occurs in about 20 percent of patients with stents. If restenosis occurs, another balloon angioplasty or stenting procedure may need to be performed.
Can restenosis be prevented?
Doctors continually try to find new ways to prevent arteries from closing again after angioplasty or stenting. In recent years, doctors have used new types of stents, some of them are coated with drugs that reduce the chance that the blood vessel closing again. These coated stents slowly release the drug into the surrounding tissue, slowing or stopping the restenosis process. Coated stents appear to show promise in enhancing the long-term success of this procedure.
Researchers are also designing smaller stents and custom-made stents, which can be inserted into smaller blood vessels. They are also designing stents for blood vessels that have many blockages, including branching blood vessels. Other stents are being coated with blood thinners to prevent blood clots from forming inside the stent. More recently, researchers have begun to develop non-metallic stents that will eventually dissolve in the artery. These stents open the artery, giving the same results as bare metal stents, but reduce the risk of restenosis because they do not remain in the artery.